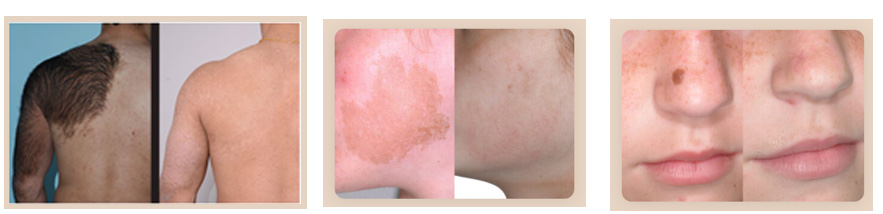
About Pigmented Birthmarks and Treatment Options
There are many different types of pigmented birthmarks, which vary in their structure, behavior, size, appearance, and anatomic location. While the vast majority of pigmented birthmarks are benign, some can be associated with abnormalities in other organ systems or can be a feature of certain genetic syndromes. It is also possible, albeit rare, for skin cancer to arise in certain types of pigmented birthmarks. For these reasons, it is not only important to have a board-certified dermatologist discuss various treatment options with you, expectations of treatment, and the possible need for ongoing monitoring, but to also conduct a thorough assessment of your general health and past medical history should you possess any of the following pigmented birthmarks.
- Café au lait spots: These are well-defined, evenly pigmented spots that classically have a color resembling “coffee in milk,” (though they can in reality range from light to dark brown, depending on a person’s skin tone). They may be present at birth but are more commonly observed to appear during early childhood. A café au lait spot will increase proportionately in size as the child grows, ultimately ranging anywhere from 1-20 cm. Because there are several syndromes that can be associated with the development of large or numerous café au lait spots, it is extremely important to be seen by one of our board-certified dermatologists, who will conduct a thorough physical exam, and obtain a detailed medical history. Some of the genetic syndromes that have been strongly associated with the presence of café-au-lait macules include neurofibromatosis, McCune-Albright, LEOPARD, Cowden, and Bannayan-Riley-Ruvalcaba.
- Nevus spilus: Also known as a speckled lentiginous nevus, this appears as small dark spots that are superimposed over a more lightly pigmented patch. Nevus spilus is usually present at birth or will become evident during the first year of life. While the vast majority of nevus spilus are solitary and benign, there is a small increased risk of melanoma arising within them, as well as a risk of their being associated with neuromuscular abnormalities, neurologic abnormalities, neurofibromatosis, and phakomatosis pigmentovascularis, among others.
- Becker nevus: This is a benign, melanocytic birthmark that appears as a large, hyperpigmented patch on the upper trunk. During puberty, it is common for a Becker nevus to darken, become slightly raised, and start to grow coarse hair. Very occasionally, there may be growth defects in the underlying tissue on the affected side (chest, arm). Becker nevus is much more common in males, but cases in females have been reported.
- Nevus sebaceous: This is usually found on the scalp, face, or neck and, as the name implies, can frequently have a somewhat greasy appearance. The birthmark itself is comprised of an increased number of oil glands, sweat glands, and hair follicles. During infancy, nevus sebaceous will usually appear as a smooth to velvety to slightly cobblestoned pink to yellow-orange hairless patch. In those with skin of color, nevus sebaceous may range from tan to dark brown to gray. During puberty, nevus sebaceous will often become darker and more raised. While the vast majority of nevus sebaceous occur in isolation and are benign, those that are very extensive or numerous have been associated with neurologic, ocular, skeletal, cardiovascular, and urologic abnormalities. Additionally, in adulthood, it is necessary to routinely monitor nevus sebaceous for any changes in appearance, as a variety of benign and malignant neoplasms, including several different types of skin cancer, have been reported to arise in them.
- Epidermal nevus: This is comprised of an overgrowth of epidermal cells that appear in a linear or whorled pattern, with a texture that can be smooth, velvety, or warty. Most of these are apparent at birth and may continue to extend or enlarge during childhood. At the onset of puberty, many epidermal nevi (plural of nevus) will become darker and thicker as a result of hormonal influences. A number of genetic mutations have been identified to be associated with epidermal nevi—some of these mutations are risk factors for cancers, and there have consequently been reports of internal malignancy occurring in individuals with extensive epidermal nevi. There is also a condition known as epidermal nevus syndrome, in which epidermal nevi are associated with central nervous system, ocular, and skeletal abnormalities.
- Nevus of Ota: This results when an increased number of melanocytes (pigment producing cells) become located in the dermis and manifest as a speckled to even toned slate gray/dark brown/black patch on the upper face. Sometimes nevus of Ota will also extend onto the mucosa of the mouth and nose, and/or onto the sclera of the eye. Cases of glaucoma have been reported in association with Nevus of Ota, as have very rare cases of melanoma of the skin, eye, and central nervous system. For this reason, it is important to establish care with an ophthalmologist. Nevus of Ota can occur in anyone, but is more common in individuals of Asian and African descent. Nevus of Ito shares many similar features with Nevus of Ota but is located in the neck and shoulder region instead.
- Congenital dermal melanocytosis (aka Mongolian spot): Like Nevus of Ota, this condition is caused by an increased number of melanocytes (pigment producing cells) in the dermis. It will appear at birth as a gray to bluish patch that is usually located on the buttocks and lower back but can also occur on other parts of the body. As in the case of Nevus of Ota, congenital dermal melanocytosis is more common in individuals of Asian and African descent but can occur on anyone. Unlike Nevus of Ota, however, most cases of congenital dermal melanocystosis will fade as the infant ages, and rarely warrant treatment as a result.
- Hori nevus: Similar to Nevus of Ota/Ito and congenital dermal melanocytosis, Hori nevus is the result of melanocytes located deeper in the dermis. However, unlike its counterparts, Hori nevus is not present at birth but instead becomes visible during late adolescence to early adulthood, most frequently on the face and more rarely on the trunk and extremities. While the manner in which Hori nevus develops is not fully understood, it is believed that dermal melanocytes are activated by some sort of trigger—such as sun exposure, hormones, inflammation—that causes the pigment to become visible.
- Congenital melanocytic nevus (CMN): This is a type of birthmark that is present at birth or becomes apparent during the first few weeks of life. Initially flat, smooth, and lighter in color, CMN will often darken during childhood, become more textually apparent, and grow thick, dark hair. Although CMN can occur anywhere on the body, it is more common on the trunk and extremities, and less common on the head and neck. CMNs can vary greatly in size—while small ones are considered to be less than 1.5 cm, it is possible for giant CMN to be larger than 60 cm and cover a significant portion of the There is an increased risk of melanoma arising in the setting of CMN, and this risk increases with the size of the birthmark. CMN may also be associated with a number of other genetic syndromes such as Carney complex, LAMB syndrome, NAME syndrome, neurofibromatosis, and others.
How are pigmented birthmarks treated?
At the Gateway Aesthetic Institute & Laser Center, we offer a wide range of treatment options for pigmented birthmarks. Our board-certified dermatologists pride themselves on taking a customized and collaborative approach to treating your unwanted pigment, which will be informed by your comfort level with various treatment options, lifestyle, medical history, skin type, and other concurrent skin issues that you are looking to address. When it comes to treating pigmented birthmarks, there is no one size fits all approach. Some of the treatment options that our board-certified dermatologists will discuss with you include:
Pigment directed picosecond lasers such as the:
- Cynosure Picosure®
- Fotona Starwalker® PQX
- Quanta Discovery® Pico
Pigment directed nanosecond (Q-switched) lasers such as the:
- Fotona Starwalker® MaQX
- Fotona QX MAX®
- Lumenis Versapulse®
Pigment directed long-pulsed lasers such as the:
- Quanta Light Evo®
- Quanta Thunder®
- Fractional lasers such as Fraxel® DUAL
- Surgical excision is also an option if the birthmark is small enough
- Fully ablative lasers such as the Fotona SP DynamisÒ
What is the recovery time following treatment of a pigmented birthmark?
The amount of time you will need to recover from treatment depends on the type of birthmark you have, it’s size, anatomic location, and the manner in which it is being treated. Broadly speaking, all birthmarks will need to be protected from the sun while they are actively being treated—this is because sun exposure has the potential to make all pigment darker, and this risk is increased following laser treatments while your skin is still red.
For birthmarks that undergo surgical excision, you should plan to be on light duty for 1-2 weeks while your sutures are in, and to not fully immerse the surgical site in water. For birthmarks that are treated with laser, the downtime is minimal in most cases, and people will usually not have to set aside any dedicated time for recovery.
The best way to determine whether your birthmark is a good candidate for treatment, the type of treatment that is most appropriate, as well as how much downtime your treatments will entail, is to have a consultation with one of our board-certified dermatologists. They can address all of your questions and concerns and work collaboratively with you to identify the best course of action for treating your pigmented birthmark.
Why trust Gateway Aesthetic Institute and Laser Center for the treatment of pigmented birthmarks?
Our board-certified dermatologists are skin care experts who understand that a pigmented birthmark can make a person feel self-conscious and be associated with painful memories of people staring curiously or saying critical things about its appearance. Our dermatologists believe that the successful treatment of a pigmented birthmark requires a customized approach that considers the type of birthmark, its physiological behavior, size, location, and risk for future malignant transformation. You can be assured that when you come to Gateway Aesthetic Institute and Laser Center to have your birthmark assessed, our board-certified dermatologists will carefully take all of these things into consideration when discussing treatment options with you. You can also be assured that our dermatologists have the most state-of-the-art lasers to treat your birthmark with, if it is determined that that is the best course of action.