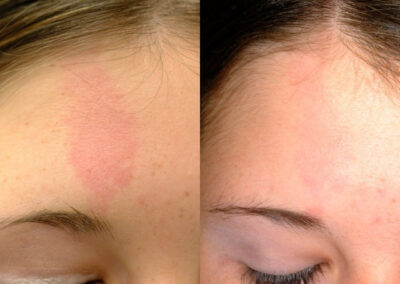
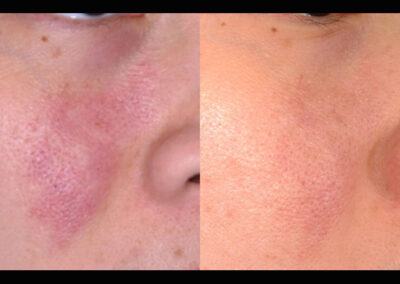
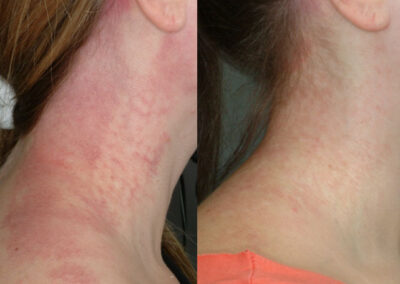
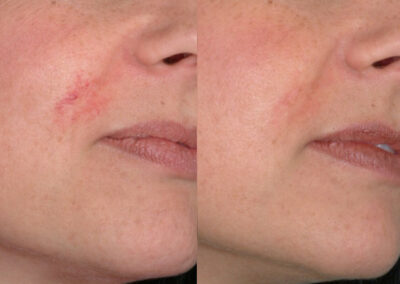
About Vascular Birthmarks and Treatment Options
There are many different types of vascular birthmarks, which vary in their structure, behavior, size, appearance, and anatomic location. While most small, solitary vascular birthmarks occur in isolation, some can be associated with abnormalities in other organ systems, or can be a feature of certain genetic syndromes when large or numerous. For this reason, it is not only important to have a board-certified dermatologist to discuss various treatment options with you, expectations of treatment, and the potential need for ongoing monitoring, but to also conduct a thorough assessment of you or your child’s general health and past medical history should any of the following vascular birthmarks be present.
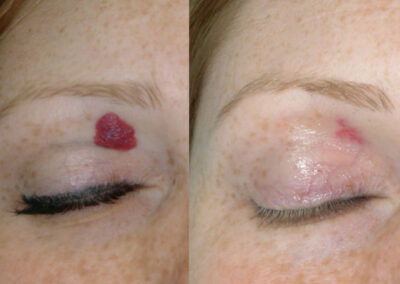
- Infantile hemangiomas: These occur in up to 10% of infants, with half of them appearing on the head and neck. They tend to grow rapidly during the first 3-5 months of life, then plateau and start to regress by 12 months. While 90% of infantile hemangiomas will completely involute by age 10, at least 30% of children will be left with scar tissue or blood vessels on the surface of the skin that serve as a reminder that it was once present. For this reason, many parents will elect to treat an infantile hemangioma early, to minimize the scarring and vascularity that can be left in its wake. Other reasons to treat an infantile hemangioma are proximity to vital facial features such as the eyes, nose, mouth, and anogenital region, as well as ulceration. An ulcerated infantile hemangioma can be very painful for an infant or child, and is also prone to bleeding and infection.
Infantile hemangiomas are that greater than 5 cm in diameter are known as segmental hemangiomas, and raise concern for the presence of other regional anatomic abnormalities. Examples of syndromes that are associated with segmental infantile hemangiomas include PHACE, LUMBAR, SACRAL, and PELVIS syndromes. These syndromes can variously affect major structures such as the eyes, heart, skeleton, spinal cord, kidneys, among many others.
- Congenital hemangiomas: As the name implies, are congenital hemangiomas are present at birth. There are, interestingly, 4 different types of congenital hemangiomas, which are differentiated by their behavior both before and after birth. Depending on the size of the hemangioma, as well as its subtype, laser or surgical excision may be treatment options. The 4 types of congenital hemangiomas include:
- RICH is a “Rapidly Involuting Congenital Hemangioma.” RICH will start to shrink during the first few weeks of life, and is usually gone by 6-14 months.
- NICH is a “Non-Involuting Congenital Hemangioma.” NICH does not regress and may actually enlarge over time.
- PICH is a “Partially Involuting Congenital Hemangioma.” PICH will partially regress in some areas, but will not regress in others.
- FICH is a “Fetally Involuting Congenital Hemangioma.” FICH will start to regress before the child is born, and will continue to do so until it is fully involuted.
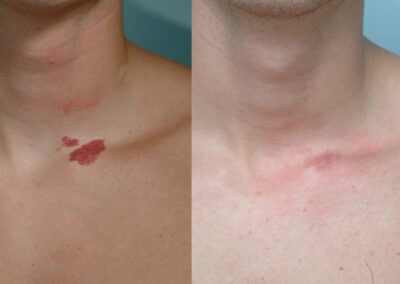
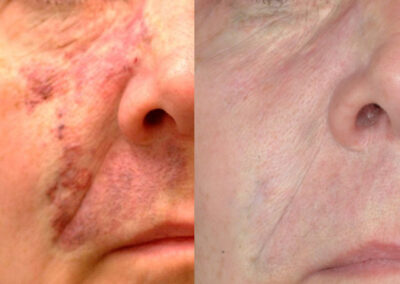
- Port-Wine Stain: This is a vascular malformation that is made out of capillaries. Port-wine stains tend to darken over time, and may also become thickened and nodular. While they can occur in complete isolation, some port-wine stains can be associated with various syndromes and anatomic abnormalities such as Sturge-Weber syndrome, Klippel-Trenaunay syndrome, phakomatosis pigmentovascularis, as well as spinal cord abnormalities. Port-wine stains on the forehead or near the eye may be associated with glaucoma and therefore warrant ophthalmologic evaluation. Laser therapy is most effective for port-wine stains when initiated at a young age.
- Nevus simplex (also known as salmon patch, stork bite, angel’s kiss): This is the most common vascular lesion seen in infants. It is a benign collection of dilated capillaries that is most commonly found on the back of the scalp/nape of the neck, as well as the central forehead, though other locations are also possible. While nevus simplex will increase in size proportionally as a child grows, those on the face tend to become less noticeable usually by 1-2 years of age.
- Tufted angioma: This is a rare vascular tumor, comprised of capillaries and lymphatic vessels, that can be present at birth or become apparent within the first 5 years of life. The behavior of tufted angiomas can vary widely—after an initial period of growth, some may spontaneously regress, some may only partially regress, and some may persist in size. They can likewise vary in the degree of severe associated complications, as some tufted angiomas are capable of causing platelet consumption, coagulopathy, and hemolytic anemia. Treatment options for a tufted angioma will depend on size, location, symptoms, associated thrombotic complications, as well as the age of the patient.
There are other rare vascular lesions that can be observed in infancy, as well as during adolescence and adulthood. Some of these lesions may be amenable to laser treatment, while some may not. If you or your child is living with a vascular lesion that has not been discussed above, our board-certified dermatologists may still be able to help you. The best way to determine the type of vascular condition you are dealing with, as well as options for treatment, is to schedule a consultation with one of our board-certified dermatologists.
How are vascular birthmarks treated?
The treatment approach for a vascular birthmark depends on many different factors, such as the size, location, age, and depth of the birthmark, what types of blood vessels it is comprised of, the patient’s ability to tolerate treatment, and what other possible health conditions or syndromes are present that are related to the existence of the birthmark. At a minimum, it is possible to use various lasers and energy-based devices to destroy the blood vessels that the birthmark is comprised of. Some of the lasers and energy-based devices that our board-certified dermatologists will use to accomplish this include:
-
-
- Fotona SP Dynamis® 1064-nm Nd:YAG laser
- Candela Vbeam® 595-nm pulsed-dye laser
- Lumenis Vasculight® intense pulsed light
- Cynosure Cynergy ® 585-nm/1064-nm laser
-
Additionally, in the case of certain birthmarks such as infantile hemangiomas, it may be necessary to initiate oral medication (propranolol), topical medication (timolol), or both to further expedite the resolution of the hemangioma. Finally, in some cases, if the birthmark is small enough, and the patient is able and willing to tolerate surgery, then surgical removal is also a treatment option to consider.
What is the recovery time following treatment of a vascular birthmark?
The amount of time that is needed to recover from treatment depends on the type of birthmark, it’s size, and anatomic location. Broadly speaking, all birthmarks will need to be protected from the sun while they are actively being treated—this is because sun exposure has the potential to cause hyperpigmentation following treatment, which can make subsequent treatments more high risk (as it increases the chance of thermal damage to the surface of the skin).
Laser treatment of vascular birthmarks commonly results in swelling, bruising, and some tenderness in the days following treatment. Usually these side effects are self-limited, and will resolve with supportive care only (such as acetaminophen as needed, and cool compresses). Very rarely, parts of the birthmark might blister and form a scab, which can prolong recovery time slightly. Despite the potential for these side effects, most people do not have to take any time away from school, work, or their personal lives in order to recover from vascular birthmark treatments.
For birthmarks that undergo surgical excision, you should plan to be on light duty for 1-2 weeks while your sutures are in, and to not fully immerse the surgical site in water.
The best way to determine whether your birthmark is a good candidate for treatment, the type of treatment that is most appropriate, as well as how much downtime your treatments will entail, it so have a consultation with one of our board-certified dermatologists. They can address all of your questions and concerns, and work collaboratively with you to identify the best course of action for treating your vascular birthmark.
Why trust Gateway Aesthetic Institute and Laser Center for the treatment of vascular birthmarks?
Our board-certified dermatologists are skin care experts who understand that a vascular birthmark can make a person feel self-conscious, and be associated with painful memories of people staring curiously or saying critical things about its appearance. Our dermatologists believe that the successful treatment of a vascular birthmark requires a customized approach that considers the type of birthmark, its physiological behavior, size, location, and possible association with other anatomic anomalies and syndromes. You can be assured that when you come to Gateway Aesthetic Institute and Laser Center to have your birthmark assessed, our board-certified dermatologists will carefully take all of these things into consideration when discussing treatment options with you. You can also be assured that our dermatologists have the most state-of-the-art lasers to treat your birthmark with, if it is determined that that is the best course of action.